Table of Content
Once you have been assessed as eligible for our services, a care coordinator will work with you to determine which services would best support your health and well-being – at home or in the community. Visit our Care Coordination page to learn more about the important role care coordinators play in Ontario’s health care system. You can also visit our Home Care page for more information about services. HomeCaring has a dedicated team of professionals with skills and experience across the Aged Care and Disability industries, we provide services through NDIS, Home Care Packages and private arrangements. We have the flexibility and knowledge to be responsive to your needs at all times.
Overcome common measurement obstacles and synthesize program data. Establishing referral partnerships to address gaps in care for palliative care patients. The National Consensus Project Clinical Practice Guidelines are the national standard for high quality palliative care.
Palliative Care in Cancer
If the doctor determines that the cancer is not responding to chemotherapy and the patient chooses to enter into hospice care, then the chemotherapy will stop. For example, if the person has high blood pressure, he or she will still get medicine for that. Increasingly, people are choosing hospice care at the end of life. Hospice care focuses on the care, comfort, and quality of life of a person with a serious illness who is approaching the end of life.
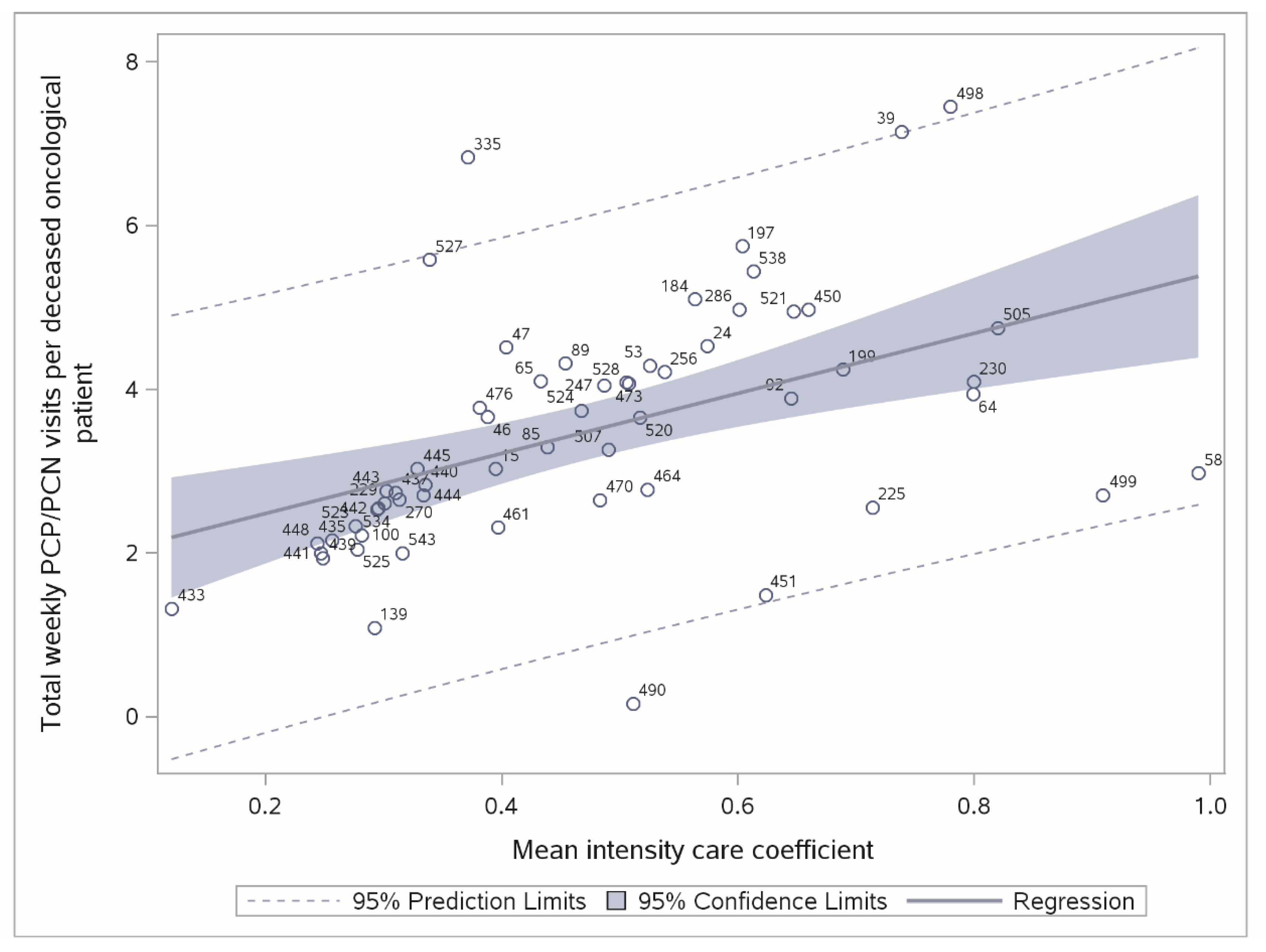
The profile program helps understand the demand for palliative care in a service. This is achieved through identifying the characteristics of those that need palliative care and the number that need it. The program allows for understanding how the needs of patients in your service change over time and service activity.
Day-to-Day Program Operations
In the United States, people enrolled in Medicare can receive hospice care if their health care provider thinks they have less than six months to live should the disease take its usual course. Doctors have a hard time predicting how long an older, sick person will live. Health often declines slowly, and some people might need a lot of help with daily living for more than six months before they die. In addition to improving quality of life and helping with symptoms, palliative care can help patients understand their choices for medical treatment.

The complex needs of these patients can be met most effectively through dedicated palliative care programs. Through ongoing, thorough communication that addresses the physical, emotional, social, and spiritual needs of patients, palliative care teams support the best quality of life possible that all patients deserve. According to the Center to Advance Palliative Care, developing a palliative care program in a hospital requires a relatively low start-up investment and can have an immediate impact. The ethical principles of nonmaleficence, beneficence, and autonomy require that hospitals better integrate the palliative care philosophy into the cure-focused health care system by developing high-quality, in-patient palliative care services.
Tell us about your care
It is my opinion that hospitals have the ethical obligation to support the provision of quality care by implementing in-patient palliative care services. Hospital palliative care services are significant in realizing that "the task of medicine is to care even when it cannot cure." Patients deserve the best quality of health care hospitals can provide at all stages of illness. The complex needs of dying patients in particular can be met most effectively through dedicated palliative care programs. Palliative care is especially suited to patients with incurable, progressive illnesses and often is centered on the needs of patients and their families at the end of life. You would want her to have the best quality of life possible.

She continued to complain of headache and shortness of breath, and the nurses noted that she was increasingly irritable and hardly slept. During the night, Mrs. Smith suffered an acute nose bleed and aspirated blood into her lungs, causing respiratory distress, and she was intubated. Once a fairly independent woman, Mrs. Smith now lay in the ICU with a spreading infection and a ventilator pumping air into her lungs to keep her alive.
Services in your home
Perhaps they wait too long to begin hospice and they are too close to death. Or, some people are not eligible for hospice care soon enough to receive its full benefit. Starting hospice early may be able to provide months of meaningful care and quality time with loved ones.

They perform well in terms of their measurement properties. Each tool has been used with hundreds of thousands of patients over the last decade. Read the new global consensus-based palliative care definition, now endorsed by 1193 individuals and 190 organizations around the world. PCSE volunteers are a compassionate, caring and dedicated group of people who support those in a very vulnerable situation.
Toolkit to support strategic planning, team leadership, and professional development for the palliative care leader. Whether your palliative care consults are triggered based on standard clinical criteria or depend upon individual referrers, collaboration is necessary. Use these tools to build, evaluate, and improve relationships with referrers. General palliative care referral criteria for children with serious illness, and for specific diseases including cancer and pulmonary, genetic, neurologic, metabolic, and other diagnoses. Identifying patients with frailty who are at high risk for health care utilization and adverse outcomes. Concise, practical, peer-reviewed and evidence-based summaries on topics important to clinicians and trainees caring for seriously ill patients.
We understand the struggles of ageing, and go beyond just providing a carer. The compassion and care you provide can have a profound effect on those you serve. Guidance on needs assessment, screening criteria selection, implementation planning, and evaluation.


No comments:
Post a Comment